Consumer Experience

Sarah Folasaitu
Sarah is pregnant with her first child. She is having her care at Westmead Hospital in Western Sydney where the team looks after women with high risk pregnancy complications. Sarah reported noticeable changes in her fetal movements, and has been monitored closely. Sarah and her care providers have agreed that an early induction of labour is necessary to reduce the risk of stillbirth. Raising awareness and improving care for women with decreased fetal movements and improving decision-making about the timing of birth for women with risk factors are two of the five elements in the Safer Baby Bundle.
Ann-Maree Imrie and her family were delighted to welcome baby Jesse. Ann-Maree’s experience with a previous pregnancy, however, turned out to be a motivating force in her life.
Ann-Maree Imrie
Ann-Maree shares her experience of stillbirth
In my first year of marriage with my husband, we decided to try for a baby, and all went pretty smoothly. We only tried to conceive for five months and then fell pregnant and we were really excited, and I guess that was our first experience. We didn’t have any other children, so we were just excited cruising along – I was really healthy. I didn’t have any issues throughout the pregnancy and obviously did all the things expecting parents do. We started planning, started purchasing baby items and the pram and clothes and things for the baby room and all of that and we were feeling sort of carefree and you know fully expecting to bring home a baby at the end. And six and a half months into the pregnancy I just noticed reduced movement and I thought – well I believed that myth that the baby, the bigger the baby gets the less room they have to move so I sort of thought it’s normal that the movements are slowing down which I’ve since found out is not right at all. Yeah, I was actually at work and I decided, because I’d noticed the previous evening that movements had reduced, and I still got up and took myself to work and I was still a bit concerned so I just popped out to the GP who was just next door from my work to get a check just fully expecting them to say yeah your fine to go back to work. They couldn’t find a heartbeat with the doppler and so sent me straight to the hospital where my husband met me and then they tried to find a heartbeat on the doppler there and they couldn’t find one and still, well at that point I guess, we started worrying but we still weren’t too panicked and then we were just told a sonographer will come in and do a scan and so I just remember him wheeling in the machine and we were just laying there. It was all pretty quick. He said I’m sorry I’m unable to find a fetal heartbeat and so my husband and I just crumpled. We weren’t expecting it at all. It was just utter shock and disbelief and we both just burst into tears and just went straight into well what now? What does this mean? What do we do and we were told well you can pick a time between now and the next seven days to come back to the hospital. We were told you can go home and come back any time in the next week and we’ll induce you and you’ll give birth and I was so shocked I remember saying to them oh I’m not doing that because I was so horrified that I would have to give birth I just couldn’t believe it and they just spoke to me about the benefits of doing so and it would be better for future pregnancies if I gave birth naturally so my husband just jumped in and said well we’ll come back tomorrow which I’m really glad he did because when we went home that evening it was just the longest night of our lives sort of laying there waiting, knowing the baby wasn’t alive and so yeah we got up the next morning, packed our bags went into the hospital and I was induced at 9 o’clock and then our little boy Xavier was born at 2.18pm.
I believed that myth that the bigger the baby gets the less room they have to move.
Ann-Maree’s experience motivated her and her husband to become ambassadors for the Stillbirth Foundation. She also wrote a children’s picture book for bereaved parents to read to their baby as a way of keeping the connection. Ann-Maree applied and was accepted as a consumer representative on the NSW Safer Baby Bundle Working Group.
I think for me personally and I’ve heard a lot of other women say that they, they kind of want to be the cool pregnant person that says no I’m fine and I don’t want to be a burden or a bother to anyone so I think that possibly leaves women worrying in isolation about things when they could be reaching out for help.
I often think this has been one of the tricky things emotionally about being part of working party is knowing this program and education pieces are out there now, I wonder, if I had of been more aware of the movements in particular would I have acted sooner and potentially saved Xavier’s life and so that makes me think if this information is getting through to women and they realise the seriousness and importance of it, then yes they will take action. Just reassuring women that they’re not a burden because I think for me personally, and I’ve heard a lot of other women say that they, they kind of want to be the cool pregnant person that says no I’m fine, I’m fine and I don’t want to be a burden or a bother to anyone so I think that possibly leaves women worrying in isolation about things when they could be reaching out for help.
The Clinical Team
The launch of the NSW Safer Baby Bundle was held at Westmead Hospital on 18 January 2020. Following the official launch, a workshop was held with key core maternity health care providers, including midwives, obstetricians and general practitioners from Western Sydney and South West Sydney local health districts.

The Safer Baby Bundle launch event at Westmead Hospital 18 January 2020.
Project Lead for the Safer Baby Western Sydney implementation is Susan Heath, High Risk Pregnancy Clinical Midwifery Consultant. Susan runs the Rainbow Mums group which supports pregnant women who have experienced a stillbirth in their first pregnancy.

Susan Heath, High Risk Pregnancy Clinical Midwifery Consultant, Westmead Hospital
Launching [the Safer Baby Bundle] was really a way of creating engagement with all those multidisciplinary teams that needed to be involved as well as letting our local community be aware. We had consumer engagement, media present as well, local media and television. It was a whole day workshop with all the key players in the care around women for prevention of stillbirth. We left that day with the key players in Stillbirth Prevention Care across the LHD up to date with the latest literature because we had the CRE come along, we had the CEC support us with the best implementation science tools that we have available as well to further the project and consumers there to remind us of who we are actually doing all this work for.
It is actually empowering for us to be able to, as clinicians who work in that field, to be actually be able to have the power of the CEC to help us implement evidence-based practice.

An extensive range of materials developed by the Stillbirth CRE are now available to pregnant women in health facilities. They included flyers and videos promoting the five elements that used together can reduce the chance of a stillbirth.
For Susan Heath, the Safer Baby Bundle program feels like the culmination of many years of work to develop better clinical practices around stillbirth. She is working towards change in clinical practice and change in community attitudes. According to Susan, “one of the big things the stillbirth CRE have done through this kind of work with the CEC is to actually get stillbirth into the public domain, which has often been a bit of a taboo so a lot of people don’t talk about stillbirth or what’s happened to them, broader strategies like this educate the wider community and that’s as important as educating the clinicians looking after the women”.
A lot of people don’t talk about stillbirth or what’s happened to them, broader strategies like this educate the wider community and that’s as important as educating the clinicians looking after the women.
CEC Program
The CEC has partnered with the Stillbirth Centre for Research Excellence, Safer Care Victoria and the Queensland Clinical Excellence Division, in a national collaborative to reduce the number of stillborn babies.
A key driver of the political advocacy has been Senator Kristina Keneally, who’s baby Caroline was stillborn 20 years ago. Seeing the growing evidence base and support from major advocacy groups, in her maiden speech in the senate she called for a national inquiry into stillbirth research and education and established a select committee to oversee the inquiry, chaired by Senator Malarndirri McCarthy. All committee members had also been affected by stillbirth.
The CRE for Stillbirth was formed in 2017 followed by development of the Safer Baby Bundle which aims to reduce the number of preventable stillbirths after 28 weeks gestation, by 20% by 2023. The Bundle has five evidence-based elements that emphasise the importance of best practice care. Reinforcing the five elements of the Bundle by providing women with midwifery continuity of care, has the potential to strengthen the Bundle’s impact and reduce the rate of stillbirth. Safer Baby Bundle focuses on improving care thorough better information and education for women during pregnancy and for maternity care providers.
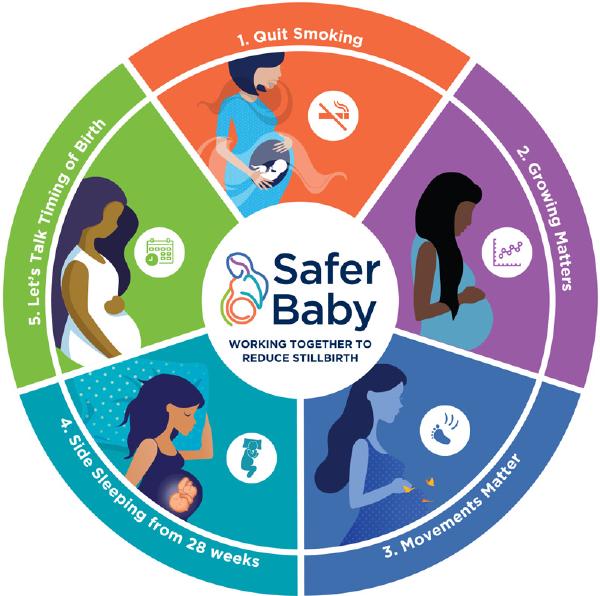
The five elements of the Safer Baby Bundle are: Supporting women to stop smoking in pregnancy, Improving detection and management of fetal growth restriction, raising awareness and improving care for women with decreased fetal movements, Improving awareness of maternal going to sleep position in late pregnancy and improving decision-making about the timing of birth for women with risk factors for stillbirth.
Safer Baby Bundle aims to reduce the number of preventable stillbirths after 28 weeks gestation, by 20% by 2023
In early 2020, the CEC worked with four Local Health Districts: Hunter New England, Central Coast, Western Sydney and South Western Sydney to provide expert support for the implementation of the Stillbirth Safer Baby Bundle in NSW.
The CEC organised workshops at: John Hunter Hospital, Westmead Hospital and Tamworth Hospital. The forums supported the districts with local implementation and provided an overview of the elements of NSW Stillbirth Safer Baby Bundle, local data and measurement strategy and training in quality improvement. The CEC has additionally worked with NSW key network groups to facilitate and support all NSW maternity services to implement the five elements of the Safer baby Bundle into routine antenatal care by 2021.
In 2020, the CEC led the redesign of FONT© training. The new program, Perinatal Safety Education comprises two educational pathways delivered through online and face to face learning. Perinatal Safety Education aligns with the Deteriorating Patient Education Program with a focus on improving the recognition, response to, and management of the deteriorating mother and deteriorating fetus. The first of the two mandatory pathways were released in April 2020.
CEC Expertise
Dr Christine Marsh is a midwife and the Improvement Lead for the Safer Baby Bundle. Before joining the CEC Chris worked for the NSW Pregnancy and newborn Services Network supporting safe delivery of Maternity and newborn care across NSW. This included providing advice on the Perinatal Advice Line to ensure women with pregnancy complications received appropriate care, in the right place, at the right time as close to home as possible. Chris has extensive experience across remote, rural, regional and tertiary maternity services as a clinician, maternity manager and midwifery consultant. Chris has a PhD awarded from the University of Canberra. Her research examined the personal experiences of women, midwives and other professionals involved in the practice of an Assumption of Care for child protection concerns of a newborn at the time of birth.
Dr Christine Marsh, Project Officer, Safer Baby Bundle
Christine Marsh reflects on the need to sustain change
I was going to be a midwife and look after mothers and babies as long as I can remember. I had to wait a while before I could do midwifery and so I specialised in paediatric care prior to that while I was waiting for my time to do my midwifery training. It’s my passion, it’s not just my work it’s what it’s all about. Having children of my own I know how important that experience is for the mother and her family and how it sets herself up, sets her up for the rest of her life really, it gives her a sense of achievement and there’s nothing like the empowerment of giving birth to a baby and achieving that so it’s really close to my heart.
Safer Baby bundle is five evidence based care programs that when used together have shown overseas that it does impact on the stillbirth rate and in England and Scotland they reduced their stillbirth rate by 20% so in Australia we have 6 stillborn babies every day and if we can save one of those babies then that’s very important for that woman and her family.
The CEC has been leading the implementation and the important thing about making change to clinical care is that we make it resilient so part of what we do at the CEC is we use quality improvement science that has shown to embed and place resilience in change so it’s important that we don’t just start off with the Safer baby Bundle then a couple of years down the track we’ve lost all of the factors that are there and we know that if we use quality improvement science we’re more likely to maintain this, the effect on the stillbirth rate in the future.
The important thing about making the change to clinical care is that we make it resilient.
Sarah Folasaitu gave birth to a healthy baby girl in November 2020.

